
Bruxism Explained: Could Jaw Clenching Be Behind Your Tinnitus?
At Markham Smile Centre, we often meet patients who come in for jaw pain, clenching, or chronic headaches — and only later mention persistent tinnitus. That connection is not accidental. The jaw joint and auditory system share anatomical space and neurological pathways. When chronic bruxism places excessive strain on the temporomandibular joint (TMJ), it can influence nearby nerves involved in sound processing.
Understanding whether your tinnitus may be somatosensory rather than purely auditory changes the direction of diagnosis and treatment. In this guide, we explain how bruxism can contribute to tinnitus, how to recognize the warning signs, and when a dental evaluation may be appropriate.
Key Takeaways
- Bruxism can contribute to tinnitus, particularly when TMJ dysfunction develops.
- The jaw joint sits close to the ear canal and shares nerve pathways with the auditory system.
- Inflammation and chronic muscle tension may influence auditory processing.
- Somatosensory tinnitus often changes with jaw movement or clenching.
- Early diagnosis and targeted treatment can reduce symptoms in appropriate cases.
Can bruxism cause tinnitus or ringing in the ears?
Patients frequently ask whether bruxism can cause tinnitus. The answer is nuanced, but yes, it can contribute, especially when chronic clenching leads to joint inflammation and muscular hyperactivity.
Bruxism places excessive strain on the temporomandibular joint and surrounding muscles. Over time, this strain may result in inflammation, joint compression, and altered nerve signalling. The TMJ is located directly in front of the ear canal, separated by only a thin bony plate. Because of this proximity, joint inflammation or biomechanical stress may influence nearby auditory structures.
Research published in Frontiers in Neuroscience, "Somatosensory tinnitus: Current evidence and future perspectives," explains how trigeminal nerve input can modulate activity in the dorsal cochlear nucleus, a key centre involved in tinnitus perception. Since the trigeminal nerve supplies the muscles used in chewing and clenching, chronic bruxism may alter sensory input reaching the auditory brainstem.
Neurological pathways
The trigeminal nerve (cranial nerve V) is responsible for facial sensation and motor control of the chewing muscles. Importantly, it interacts with brainstem nuclei that process auditory signals. When jaw muscles remain in a state of prolonged contraction, trigeminal signalling may increase and influence auditory processing centres.
This helps explain why some patients notice that their tinnitus changes when they clench their teeth, move their jaw side to side, or apply pressure to facial muscles. These characteristics are typical of somatosensory tinnitus, a subtype influenced by musculoskeletal input rather than by inner ear damage alone.
Somatosensory tinnitus
Unlike primary tinnitus caused by hearing loss or noise exposure, somatosensory tinnitus often fluctuates with movement or muscle activation.
Common features include:
- Tinnitus that changes with jaw movement
- Increased ringing during stress-related clenching
- Ear fullness accompanied by jaw discomfort
- Clicking or popping sounds in the TMJ
The Journal of Oral Rehabilitation reports a significant association between temporomandibular disorders (TMD) and tinnitus symptoms. Clinically, this overlap is frequently observed in patients presenting with enamel wear, muscle tenderness, and TMJ clicking.
Dr. Amir Guorgui, BSc, DMD, MACSD adds:
"Chronic clenching places sustained pressure on the temporomandibular joint and surrounding musculature. Over time, inflammatory and neural responses may influence adjacent auditory structures."
How are bruxism and tinnitus connected anatomically?
The connection between bruxism and tinnitus becomes clearer when examining the structural relationship between the jaw joint and the ear.
The temporomandibular joint connects the mandible to the temporal bone of the skull and sits directly anterior to the external auditory canal. The auriculotemporal nerve, a branch of the trigeminal nerve, supplies both the TMJ and parts of the ear. Because of this shared innervation, joint inflammation or mechanical stress may influence auditory perception.
Data from the American Academy of Orofacial Pain indicate that approximately 30–60% of patients with TMD report otologic symptoms, including tinnitus. While this does not confirm direct causation in every case, the association is clinically significant.
TMJ dysfunction and ear symptoms
Temporomandibular disorders may present with:
- Ringing in the ears
- Ear fullness or pressure
- Headaches, particularly in the temples
- Jaw pain or stiffness
- Clicking or popping during jaw movement
Referred symptoms are common in the head and neck. The brain does not always precisely localize sensory input, which means jaw inflammation can sometimes be perceived as ear-related discomfort.
Anatomical comparison table
| Structure | Primary Function | Effect of Bruxism | Potential Auditory Impact |
|---|---|---|---|
| Temporomandibular Joint (TMJ) | Jaw movement | Overloaded by clenching | Inflammation near the ear canal |
| Trigeminal nerve | Facial sensation & motor control | Hyperstimulation from muscle tension | Modulates auditory brainstem centres |
| Dorsal cochlear nucleus | Auditory signal integration | Receives somatosensory input | May amplify tinnitus perception |
| Masticatory muscles | Jaw stabilization | Chronic contraction | Sustained neural stimulation |
This structural and neurological overlap explains why addressing bruxism can sometimes reduce the severity of tinnitus.
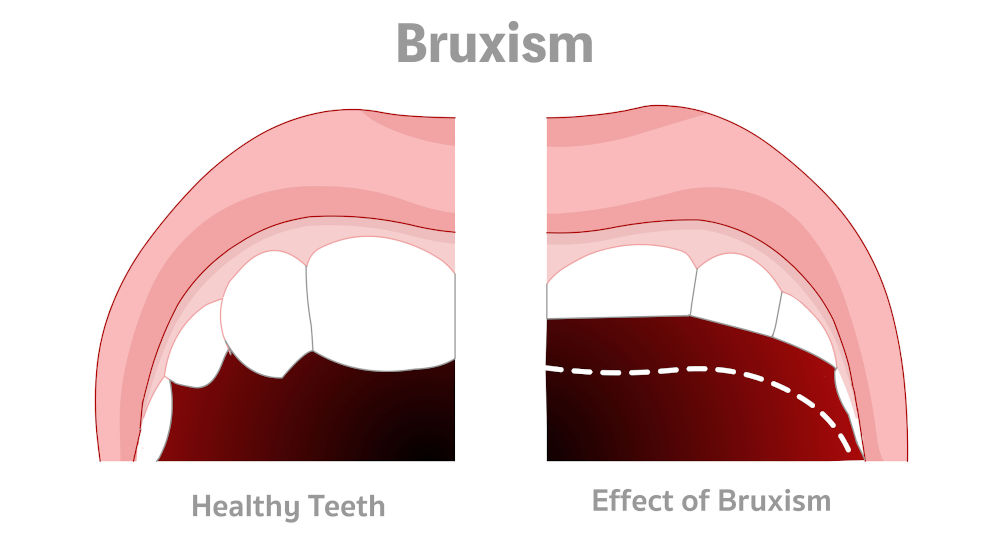
What are the symptoms of teeth grinding and tinnitus?
Teeth grinding and tinnitus rarely appear in isolation. It is typically accompanied by musculoskeletal symptoms.
Common signs include:
- Morning jaw soreness or stiffness
- Temple headaches
- Ear fullness without infection
- Audible TMJ clicking
- Tinnitus that fluctuates with clenching
According to the National Institute on Deafness and Other Communication Disorders, primary tinnitus is most often linked to auditory system damage. In contrast, somatic tinnitus frequently changes with movement or pressure — an important diagnostic distinction.
How is bruxism-related tinnitus diagnosed by a dentist?
Diagnosis begins with a comprehensive history and clinical examination.
Step-by-step diagnostic guide
- Assessment of jaw mobility and joint sounds
- Palpation of the masticatory muscles for tenderness
- Bite analysis to detect occlusal imbalance
- Identification of enamel wear facets
- Imaging (panoramic X-ray or CBCT) when indicated
- Referral to an ENT specialist to rule out primary auditory causes
Diagnostic specification table
| Diagnostic Tool | Purpose | Clinical Insight |
|---|---|---|
| Occlusal analysis | Evaluate bite forces | Detect uneven pressure distribution |
| Wear facet inspection | Identify grinding | Confirm chronic bruxism |
| Muscle palpation | Assess tension | Identify myofascial involvement |
| Imaging | Evaluate joint structure | Detect degeneration or displacement |
| ENT collaboration | Exclude ear pathology | Clarify differential diagnosis |
Differential diagnosis ensures that hearing loss, Ménière’s disease, vascular disorders, or neurological conditions are not overlooked.
What treatment options help reduce bruxism and tinnitus symptoms?
Treatment focuses on reducing mechanical load and calming neuromuscular hyperactivity.
Common interventions include:
- Custom night guards
- Occlusal splints
- Physiotherapy for jaw and neck muscles
- Stress management strategies
- Botox injections in selected cases
- Bite correction when clinically indicated
Research from the Journal of Prosthetic Dentistry supports the use of occlusal splints for reducing TMD-related symptoms. Tinnitus improvement varies but may occur in patients with somatosensory involvement.
Comparing treatment effectiveness
| Treatment | Primary Goal | Evidence Strength | Impact on Tinnitus |
|---|---|---|---|
| Night guard | Reduce grinding load | Strong for TMD | Moderate benefit when somatic |
| Physiotherapy | Decrease muscle tension | Moderate | Helpful when muscular |
| Botox | Reduce hyperactivity | Emerging | May reduce severity |
| Bite correction | Improve occlusion | Case-dependent | Variable |
| Stress management | Reduce clenching triggers | Strong behavioural evidence | Indirect benefit |
How does TMJ dysfunction increase the risk of tinnitus?
TMJ dysfunction increases the risk of tinnitus through inflammation, mechanical compression, and altered neural input.
Epidemiological studies suggest that TMD affects approximately 5–12% of the population, with higher prevalence among women. Among those diagnosed with TMD, ear-related symptoms are commonly reported.
Mechanism overview table
| Mechanism | Description | Potential Auditory Impact |
|---|---|---|
| Joint inflammation | Swelling of the TMJ capsule | Irritation of adjacent nerves |
| Disc displacement | Mechanical stress within the joint | Altered sensory feedback |
| Muscle hyperactivity | Chronic contraction | Increased trigeminal signalling |
| Central sensitization | Heightened neural response | Amplified tinnitus perception |
Dr. James C.H. Ko explains:
"When TMJ inflammation becomes chronic, surrounding neural pathways may become sensitized. That sensitization can influence how auditory input is processed."
What lifestyle changes can reduce teeth grinding and protect your hearing?
Daily habits significantly influence bruxism severity.
Step-by-step prevention guide
- Reduce caffeine intake, especially in the evening
- Maintain consistent sleep hygiene
- Practice stress-reduction techniques such as diaphragmatic breathing
- Improve posture during computer work
- Perform guided jaw stretching exercises
- Avoid excessive gum chewing
Chronic stress is a major contributor to clenching. Improved sleep quality can reduce nocturnal muscle activity. Postural correction reduces strain on jaw and cervical muscles, potentially decreasing somatosensory input to auditory centres.
When should you seek professional help for bruxism and tinnitus?
Occasional jaw tension or temporary ringing may not require urgent care. However, certain symptoms warrant professional evaluation.
Red flags
- Persistent tinnitus lasting several weeks
- Sudden hearing loss
- Severe or worsening jaw pain
- Locking of the jaw joint
- Dizziness or balance disturbances
- Neurological symptoms accompanying tinnitus
The National Institute on Deafness and Other Communication Disorders advises immediate medical evaluation for sudden hearing changes.
An ENT specialist evaluates hearing thresholds, vestibular function, and potential inner ear disorders. A dentist trained in TMD assesses occlusal imbalance, wear facets, joint mechanics, and muscle hyperactivity. Early intervention improves the likelihood of symptom stabilization.
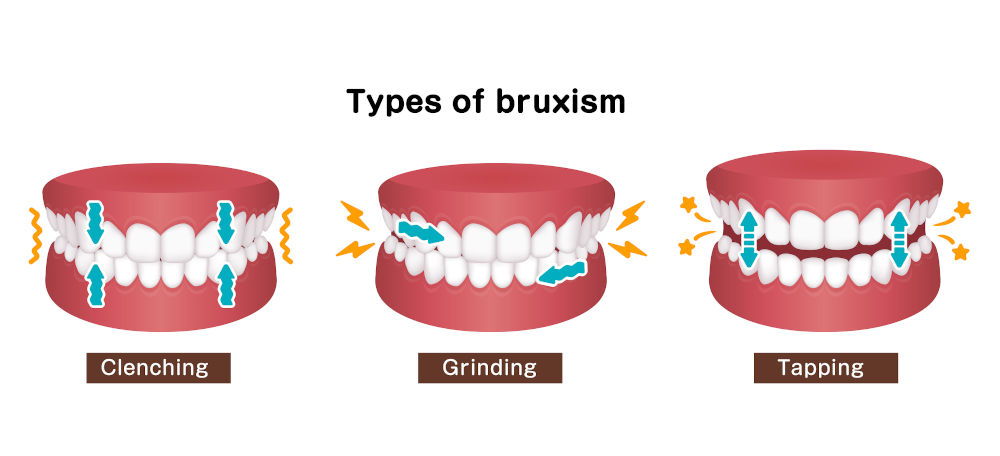
What should you know about the link between bruxism and tinnitus?
The link between bruxism and tinnitus is grounded in shared anatomy and neural pathways. While not all tinnitus originates from jaw dysfunction, somatosensory forms may be influenced by chronic clenching, inflammation, and muscle tension.
When tinnitus fluctuates with jaw movement, occurs alongside TMJ symptoms, or is accompanied by visible enamel wear, a dental evaluation should be considered.
Summary table
| Key Finding | Clinical Meaning |
|---|---|
| TMJ and ear structures share nerve pathways | Jaw dysfunction may influence auditory perception |
| 30–60% of TMD patients report ear symptoms | Strong clinical association |
| Somatosensory tinnitus changes with movement | Suggests musculoskeletal involvement |
| Early intervention improves outcomes | Reduces risk of chronic sensitization |
At Markham Smile Centre, a comprehensive assessment helps determine whether bruxism contributes to tinnitus symptoms. Identifying and managing the underlying mechanical and behavioural factors provides patients with a structured, evidence-informed path forward.
Frequently Asked Questions
1. Can bruxism really cause tinnitus?
Yes, bruxism can contribute to tinnitus in certain cases, particularly when it leads to TMJ inflammation and muscle tension. This form is often classified as somatosensory tinnitus, which may change with jaw movement.
2. How do I know if my tinnitus is jaw-related?
If your tinnitus intensity changes when you clench your teeth, move your jaw, or press on facial muscles, it may have a musculoskeletal component. A dental evaluation can help determine whether TMJ dysfunction is involved.
3. Can a night guard reduce tinnitus?
A custom night guard may reduce jaw strain and muscle tension. In patients with bruxism-related tinnitus, this can sometimes reduce symptom intensity, although results vary.
4. Should I see a dentist or an ENT first?
If tinnitus is accompanied by sudden hearing loss, dizziness, or neurological symptoms, an ENT should be consulted immediately. If symptoms fluctuate with jaw movement or are accompanied by jaw pain, a dentist trained in TMJ assessment may be appropriate.
5. Is tinnitus from bruxism permanent?
Not necessarily. When bruxism is treated early and inflammation is reduced, some patients experience partial or significant improvement in symptoms.
6. What treatments are most effective for bruxism-related tinnitus?
Treatment may include occlusal splints, physiotherapy, stress management, and, in select cases, Botox. Effectiveness depends on whether the tinnitus has a somatosensory component.
References
- Frontiers in Neuroscience. Somatosensory tinnitus: Current evidence and future perspectives. https://www.frontiersin.org/articles/10.3389/fnins.2017.00207/full
- National Institute on Deafness and Other Communication Disorders. Tinnitus. https://www.nidcd.nih.gov/health/tinnitus
- Journal of Oral Rehabilitation. https://onlinelibrary.wiley.com/journal/13652842
- Journal of Prosthetic Dentistry. https://www.journals.elsevier.com/journal-of-prosthetic-dentistry
- American Academy of Orofacial Pain. https://aaop.org

See what our patients are saying:
Everyone here is very friendly and provides excellent care. I received a full exam on my first visit, and everyone took time to answer my questions and ensured I felt comfortable the entire time - exactly what you want when visiting the dentist. I highly recommend Markham Smile Centre for anyone looking for great dental care.
There is an ample parking space before you get into the office. The receptionists welcome us friendly with proper COVID-19 procedures in place. The staff worked with patient very patiently and professionally. My teeth cleaning was done by Ying, she explained every detail to me and I did not feel any pain or uncomfortable at all. Thanks to the best team !
It's been a while since I've been to a dentist but I'm trying to get back on track with health in general. Overall it was great going to Markham Smile Centre! The receptionist (I believe she was Kim) was friendly. The hygienist, Ying, was attentive and gentle during the cleaning; x-ray tech (forgot her name, sorry!) was great too. Dr. Sara Riad explained things with good detail. Looking forward to going back!
I was someone who was nervous and anxious about visiting the dentist, but the team at Markham Smile Centre has made me feel SO comfortable. Kim is so patient and helpful and Dr. Hwang and Rory are both so professional and wonderful. They thoroughly explain the procedure to make you comfortable beforehand and are very gentle. I now look forward to visiting the dentist!
I found this place on a whim when I was looking for a new dentist in Markham. My hygienist ying was super nice and her cleaning was very gentle yet thorough. I saw Dr.Jason and he was very nice and informative in regards to what needs to be done and provided me with all the information I needed to make a choice. Would recommend this place to anyone looking for a new dentist, they’re accepting new patients!!
I have been to many dentists in my life, Dr. Jason is easily the best dentist I have ever been too. He does everything he can to make you comfortable no matter the procedure and is a true professional, as does all the staff at Markham Smile Centre. Truly an amazing dentistry
The clinic was clean and the staff was very polite. I particularly liked the fact that everything was explained to me before going in for the procedure so I knew what to expect at each step. The dental hygienist who did the cleaning for me was also very gentle and took my concerns into consideration. I will definitely recommend them.
Upon arriving to the Markham Smile Centre, my son and I were greeted with a warm welcome by the receptionists. The hygienists and Dentist were very gentle and transparent with what they were doing. The hygienist that worked on my 9 year old son was patient and very friendly with him, which helped ease his nerves. Our overall experience was A+.
Since I was little, I have always hated going to the dentist... Its always uncomfortable and unpleasant. These days, visiting the dentist isn’t so bad! Dr Jason, Rory, and the lovely staff at reception make the experience 100x better. I have had absolutely no issues with the gum graft and cleanings that I’ve gotten done here. Everyone is incredibly friendly and helpful, even when I’m calling in or emailing a hundred questions :). I would highly recommend Markham Smile Centre.
Love this place! All the staffs are friendly and Professional and I mean all, cause I've been to most of their office, Markham , Stouffville, North York, and Maple. Dr. Ko is very professional and patient. Whenever I have questions and concerns he would always reply me . I would say this this dental office take care of you all the way. I would highly recommend everyone to come here for any dental works. =)

